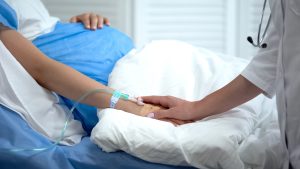
 Flushing Hospital Medical Center’s New Beginnings unit provides the women in our community and their families with the ultimate birthing experience. Each month, we cover a new topic exploring an important aspect of health and well-being for expectant mothers. This month, we’ll discuss some of what you need to know about cesarean birth (also known as a C-section).
Flushing Hospital Medical Center’s New Beginnings unit provides the women in our community and their families with the ultimate birthing experience. Each month, we cover a new topic exploring an important aspect of health and well-being for expectant mothers. This month, we’ll discuss some of what you need to know about cesarean birth (also known as a C-section).
During a C-section, your baby is delivered through incisions made in your abdomen and uterus. This happens when the health risks of vaginal delivery are too significant for either yourself or your baby. It can be planned ahead of time if:
- You experience serious medical conditions that could worsen with a vaginal birth
- You’ve had a previous C-section
- You’re expecting multiple babies
- Your baby’s exit from the cervix is obstructed
- Your baby is in an abnormal position in your uterus
Even if these factors do not apply to you, unforeseen circumstances can occur that make a C-section necessary for safely delivering your baby, such as when:
- You experience prolonged labor
- Your baby develops an irregular heart rate
- The umbilical cord compresses your baby’s head, neck, or body, or comes out of the cervix before the baby
- The placenta separates from the wall of your uterus, preventing your baby from receiving oxygen and nutrients
Flushing Hospital’s New Beginnings unit offers spacious, modern delivery suites and advanced postpartum care, providing you with a safe environment to give birth and comprehensive follow-up medical support for you and your baby. To learn more about the unit, including accommodations and services provided, please call us at (718) 670-5702.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.