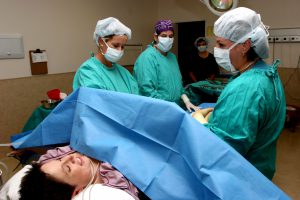
In the field of obstetrics and gynecology, there is no more debatable topic than the increased rate of cesarean (C-section) deliveries. The C-section rate is the percentage of all births that take place surgically, whereby a baby is delivered via an incision on the abdomen. Over the last few decades, this rate has increased tremendously. Up to the 1970’s, the rate of cesarean in the U.S. was less than 5% but in the subsequent few years, it climbed to 33%.
While the cesarean delivery has become a safer operation than it used to be, it is still a major abdominal surgery which should be avoided when a vaginal delivery is an option for both baby and mother. Sadly, rates of complications such as cerebral palsy have not decreased much despite the 600% increase of cesarean deliveries in the last three decades. So why then, has the cesarean rate climbed so much?
There are several factors explaining the increase the cesarean rates and there is no single answer. because so much has changed in the last two of three decades, in terms of medical, social and legal aspects. Let’s look at a few factors:
- Breech babies: Few doctors deliver breech babies vaginally because recent studies suggested that C-section births are less risky for them.
- Fewer patients attempt a VBAC (vaginal birth after cesarean): Women with a previous C-section are either not interested or not encouraged in having a vaginal birth after cesarean. There are risks involved in attempting a VBAC, but very often, they can be minimized by close fetal surveillance in labor.
- Less patience for prolonged labor: Although 24-48 hour labors are often ultimately rewarded by a natural birth, many women prefer to have a cesarean now as opposed to waiting several more hours for a possible natural birth. Sometimes, it’s best to let nature do its work and wait, but physicians and women are often impatient, not tolerant of long (but natural) labor.
- C-section delivery has become a much safer operation than it used to be decades ago: Long-term complications or serious short- term complications remain rare. This is mainly attributed to proper use of antibiotics, better and safer anesthesia techniques, and safe blood banking.
- Women wait longer to have children: Increasing age is linked to a higher risk of developing complications such as high blood pressure, placenta previa and diabetes, just to name a few. These conditions increase the risk of cesarean.
- More multiple births: The rates of twins and triplets have increased by 200-300%. 3-5% of all pregnancies are now twins (or triplets) as opposed to 1% years ago. These high risk pregnancies are associated with a much higher risk of cesarean. The majority of twin pregnancies and nearly all triplets are born via cesarean.
- Cesarean delivery on maternal request: Some women feel that women should be entitled to make decisions about their body, and about how they want to deliver and at times, women ask for a cesarean delivery In the absence of a medical indication.,
The WHO (World Health Organization) has been advocating since 1985 to reduce the C-section to10-15 percent since 1985. Here are some tips for women who want to achieve this goal and reduce their chances of having a C-section.
- Don’t be tempted to have a “scheduled” induction: while sometimes, labor inductions are medically necessary to prevent an adverse maternal or fetal outcome, many physicians and patients are tempted to “schedule” a delivery at a set time, without a medical reason.
- If your baby is breech (baby’s bottom is down instead of the head): attempt an external version. A simple procedure called External Cephalic Version may turn the baby from breech position to head down, simply by turning the baby externally, by an experiences obstetrician.
- Be patient. Labors can be long, sometimes very long, so be prepared for it and be patient. Bring a good book, movies, music and try to rest when you can (this is especially possible when you have a well working epidural).
- Bring a coach: Having a supportive person during your labor (your spouse, your mother or a trained labor coach, called a Doula) has been shown to decrease the risk of cesarean and also to improve your perception of labor. They will keep you distracted during the often very long process.
- Good life habits: women who are physically fit and are within their ideal body weight are less likely to develop diabetes, high blood pressure and excessively large babies during their pregnancy. So if you have healthy life habits, keep up with them! There is no reason to stop exercising during your pregnancy.
- Don’t eat excessively: your baby is a magnet for the calories you ingest, so there’s no reason to eat excessively to feed your baby. Don’t believe your mother, aunts or anyone else who force you to eat in order to have a big baby and tell you that “a big baby is healthier”. It simply isn’t true. Six pounds babies are just as healthy as a ten pound ones.
All content of this newsletter is intended for general information purposes only and is not intended or implied to be a substitute for professional medical advice, diagnosis or treatment. Please consult a medical professional before adopting any of the suggestions on this page. You must never disregard professional medical advice or delay seeking medical treatment based upon any content of this newsletter. PROMPTLY CONSULT YOUR PHYSICIAN OR CALL 911 IF YOU BELIEVE YOU HAVE A MEDICAL EMERGENCY.